
Last updated: Mar 9, 2026
When breakouts keep showing up along your jawline and chin, follow a predictable cycle, and resist everything you throw at them, it is worth asking whether hormones might be behind them.
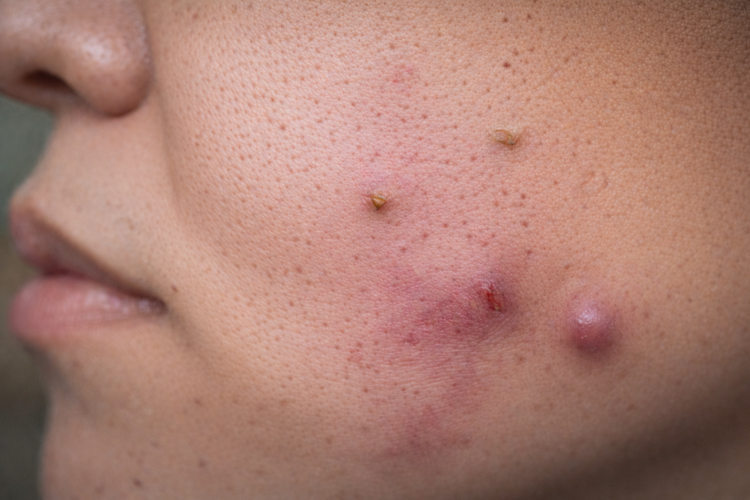
Hormonal acne behaves differently from other types of acne, and
understanding the difference can save you months of trying treatments that do not address
the real trigger.
Hormonal acne is a common reason adults experience breakouts well beyond their teenage
years, affecting both women and men across different life stages. It often looks like
regular acne on the surface, which leads many people to treat the symptoms without
addressing what is actually driving them.
Once you understand whether hormones may be involved, you can move towards treatments that
target the root cause, not just what shows up on your skin.
What Is Hormonal Acne?
Hormonal acne is caused by fluctuations in hormone levels rather than external
factors such as poor hygiene or surface bacteria alone.
Unlike typical teenage acne, which often
resolves on its own, hormonal acne can persist into adulthood and tends to follow a cyclical pattern
linked to hormonal changes.
It most commonly appears as deep, inflamed bumps along the jawline, chin, and lower face, and can
range from mild papules to severe cystic or nodular
lesions that sit beneath the skin.
What Causes Hormonal Acne?
Hormonal acne develops when fluctuations in hormones, particularly androgens such as testosterone
and dihydrotestosterone (DHT), stimulate the sebaceous glands to produce excess oil, which
combines with dead skin cells to clog pores and create conditions where acne-causing
bacteria trigger inflammation.
Several factors can contribute to these hormonal fluctuations.
Menstrual Cycle
Hormone levels shift throughout the menstrual cycle, influencing oil production in the skin.
In the week before menstruation, progesterone and oestrogen levels fall, creating a relative
increase in androgen activity that stimulates sebum production and makes breakouts more
likely.
This is why many women notice acne flaring in the same pattern each month.

Polycystic Ovary Syndrome (PCOS)
PCOS is associated with chronically elevated androgen levels, which stimulate excess oil production and contribute to persistent breakouts. If your acne occurs alongside irregular periods, weight changes, or thinning hair, PCOS may be a contributing factor worth discussing with your doctor.
Pregnancy
Pregnancy causes rapid hormonal shifts, particularly in the first trimester, as progesterone levels rise to support pregnancy. These changes can increase oil production, making breakouts more likely and sometimes more inflamed or persistent due to heightened skin sensitivity during this period.
Perimenopause and Menopause
During perimenopause and menopause, declining oestrogen levels create a relative increase in androgen influence. This hormonal shift can stimulate oil production and lead to breakouts, even in women who have not experienced acne for many years.
Testosterone Fluctuations
In men, hormonal acne is primarily driven by testosterone and DHT, which directly stimulate the sebaceous glands. Levels surge during puberty and may fluctuate in adulthood due to factors such as ageing and testosterone replacement therapy (TRT). Because these changes do not follow a predictable monthly pattern, hormonal acne in men can be harder to recognise.

Stress
Chronic stress raises cortisol levels, which can increase androgen activity and stimulate oil production. Breakouts often worsen during periods of sustained pressure, poor sleep, or emotional strain.
Medications
Certain medications can trigger or worsen hormonal acne by altering hormone levels or increasing androgen activity. These include corticosteroids, some hormonal contraceptives, and anabolic steroids.
Genetics
A family history of acne increases your likelihood of developing hormonal acne. Genetic factors influence how sensitive your sebaceous glands are to androgens and how your skin responds to hormonal fluctuations.
How to Identify Hormonal Acne
Hormonal acne has distinct patterns that set it apart from other forms of acne, making it possible to recognise the condition based on its presentation.
- Location – Breakouts typically appear along the jawline, chin, and lower cheeks, where sebaceous glands are more sensitive to androgens. Acne concentrated on the forehead or upper face is more often linked to other causes.
- Timing – Flares that occur in a predictable monthly pattern or during hormonal shifts such as pregnancy or perimenopause suggest a hormonal trigger.
- Appearance – Lesions are often deep, tender bumps beneath the skin rather than surface-level whiteheads or blackheads, and they may heal more slowly with a higher risk of scarring.
- Response to standard products – If your acne does not improve with over-the-counter treatments such as benzoyl peroxide or salicylic acid, a hormonal component may be involved.
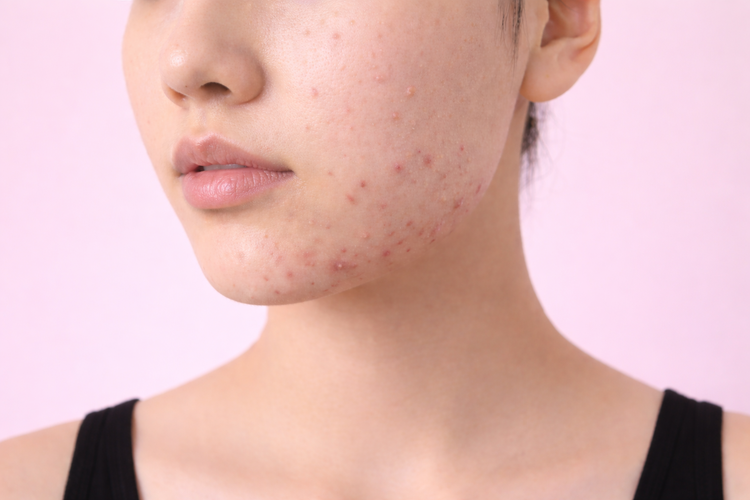
Hormonal Acne vs Other Types of Acne
Hormonal acne differs from bacterial and fungal acne in its underlying cause, typical location, pattern of flare-ups, and appearance.
| Feature | Hormonal Acne | Bacterial Acne | Fungal Acne |
|---|---|---|---|
| Primary cause | Hormonal fluctuations, particularly androgen influence | Follicular blockage with C. acnes proliferation | Malassezia overgrowth (fungal folliculitis) |
| Typical location | Jawline, chin, lower face | T-zone, forehead, cheeks | Chest, back, forehead |
| Appearance | Deep, tender nodules or cysts | Whiteheads, pustules, blackheads | Uniform, itchy small bumps |
| Pattern | Cyclical, linked to hormonal events | Persistent without cyclical pattern | Often worsens with heat and humidity |
WhatsApp Us Now
Hormonal Acne Treatment Options
Treating hormonal acne typically involves addressing hormonal causes while reducing
inflammation and preventing pore blockage.
The most suitable approach depends on acne severity, medical history, and associated conditions such
as PCOS.
| Treatment | How It Works | Typically Recommended For |
|---|---|---|
| Topical Treatments | ||
| Topical retinoids (tretinoin, adapalene) | Increase skin cell turnover, prevent pore blockage, and reduce inflammation. | Mild to moderate hormonal acne. May be combined with oral treatment. Breakouts may temporarily worsen in the first few weeks as the skin adjusts. |
| Benzoyl peroxide | Reduces acne-causing bacteria and helps unclog pores. | Mild acne or combination therapy. |
| Azelaic acid | Reduces inflammation and improves post-inflammatory pigmentation. | Sensitive skin or during pregnancy, where retinoids are not recommended. |
| Oral Medications | ||
| Spironolactone (anti-androgen) | Blocks androgen receptors in sebaceous glands, reducing oil production. | Women with moderate to severe hormonal acne. Not suitable for men or during pregnancy. |
| Combined oral contraceptives | Regulate hormone levels and reduce circulating androgens. | Women with acne linked to menstrual cycles. |
| Oral antibiotics | Reduce inflammation and the growth of acne-causing bacteria. | Short-term use alongside other treatments. Does not address the hormonal driver. |
| Isotretinoin | Significantly reduces sebaceous gland activity and oil production. | Severe or treatment-resistant acne. Requires close monitoring and strict contraception. |
| In-Clinic Procedures | ||
| Cortisone injections | Involve injecting a small amount of corticosteroid directly into inflamed cystic lesions to rapidly reduce swelling and pain. | Large, inflamed cysts requiring rapid relief. |
| Chemical peels | Use controlled chemical exfoliation (such as salicylic or glycolic acid) to remove dead skin cells, reduce pore blockage, and improve overall skin texture. | Persistent breakouts or post-acne texture concerns. |
| LED light treatment | Uses specific wavelengths of light to reduce inflammation and target acne-related bacteria within the skin. | Mild to moderate inflammatory acne. |
How You Can Support Hormonal Acne Treatment at Home
While medical treatment addresses hormonal drivers, certain skincare, lifestyle, and dietary habits can support improvement and reduce flare-ups:
- Skincare — Use a gentle, non-comedogenic cleanser and moisturiser to avoid irritation and pore blockage. Apply broad-spectrum sunscreen when out in the sun for prolonged periods of time. Avoid heavy oil-based make up that may worsen clogging.
- Lifestyle — Manage stress through regular physical activity, adequate sleep, and relaxation techniques, as elevated cortisol can increase androgen activity and oil production.
- Diet — Limit high-glycaemic foods and excessive dairy intake, which may worsen breakouts in some individuals. Include omega-3 and zinc-rich foods as part of a balanced diet to support overall skin health.
These measures can support medical treatment but are not sufficient on their own for moderate to severe hormonal acne.
Hormonal Acne Treatment Price in Singapore
At Medical Aesthetics, we offer treatment for hormonal acne and other forms of acne. Our consultation and treatment fees are as follows:
| Treatment | Price* |
|---|---|
| Consultation | From $38.15 to $70.85 |
| Retinoid | From $21.80 |
| Benzoyl Peroxide | From $32.70 |
| Antibiotic Gel | From $38.15 |
| Cortisone Injection | From $109 |
| Oral Antibiotics | From $2.40 / tablet |
| Chemical Peel | From $114.45 |
| LED Light Treatment | From $87.20 |
| Fractional CO₂ Laser | From $436 |
| Laser Soft Peel | From $436 |
*Prices are NETT and inclusive of GST.
All patients are required to undergo a consultation with our doctor to assess his or her
suitability for the relevant treatment(s).

— Dr Robert Ong
Where Can I Find Hormonal Acne Treatment in Singapore?
Book Hormonal Acne Treatment
Book Now
Enquire More Through Email
Email Us Now
Enquire More Through WhatsApp
WhatsApp Us Now
The Medical Aesthetics Track Record
Patients Consulted Since 2002
Years of Experience
Google Reviews
Experienced & Friendly Doctor
Dr Robert Ong listens attentively to your concerns and patiently discusses with you the appropriate treatment options, based on over 20 years of medical and aesthetics experience.
Affordable Treatments
We are priced competitively and affordably. We also have a variety of treatment options depending on your budget and requirements.
Safe & Effective Results
Our treatment options are safe, effective and promotes natural healing for your skin. We strive to keep your experience a comfortable one and will minimize any pain or discomfort, if any.
